You’ve paid for a hair transplant — the surgery may have taken hours, but the next few weeks are what will determine whether those grafts live, take root and deliver the density you expect. That’s the blunt message from Dr. Emrah Cinik in a recent article summarizing five common post‑op mistakes patients make, and it’s a message worth treating seriously: the hair restoration field is booming, techniques like FUE dominate practice, and adjuncts such as PRP and experimental exosome treatments are widely discussed — but evidence, regulation and aftercare protocols vary widely.
The hair restoration market is expanding rapidly: one prominent industry forecast values the global hair transplant market at about US$5.12 billion in 2022, projecting growth to US$23.32 billion by 2030 — a compound annual growth rate in the low‑to‑mid double digits over the forecast window. These figures reflect growing demand, new non‑scalp transplant applications (beard, eyebrow), and an expanding portfolio of adjunctive therapies. Market forecasts are inherently contingent on assumptions about adoption, pricing and regulation, so they should be interpreted as directional rather than definitive. The International Society of Hair Restoration Surgery (ISHRS) practice data shows notable shifts in patient behavior and technique preference: FUE is the dominant surgical approach for many practices, body and facial transplants (beard, eyebrow) are increasing, and about 25% of new patients in a recent ISHRS member survey said the “Zoom effect” (being more camera‑conscious during the pandemic) influenced their decision to seek treatment. The ISHRS census also documents the fast adoption of nonsurgical adjuncts (finasteride, topical minoxidil, PRP) and a growing awareness among patients to prioritize surgeon qualifications. Against that backdrop of rapid growth and innovation, the post‑operative window — the days to weeks after surgery — is fragile. Surgeon advice, patient compliance, and the choice of adjunct therapies can meaningfully affect graft survival and the final cosmetic result. The following sections summarize the five “never do” items highlighted by Dr. Emrah Cinik, expand on the clinical evidence where available, and provide a journalist’s critical appraisal of the strengths, gaps and risks behind the advice.
Important note: market forecasts and evolving therapies change quickly — projections like the Insight Partners’ 2030 market figure are useful industry benchmarks but not clinical guidance; experimental biologic treatments such as exosomes remain under study and are not standardized or (in most cases) regulatory‑cleared for hair restoration. Always discuss individual care with a board‑qualified surgeon and confirm any adjunct therapies with peer‑reviewed evidence or an IRB‑approved clinical trial before proceeding.
Source: WorldHealth.net Top Hair Surgeon Reveals: 5 Things You Should Never Do After a Hair Transplant - WorldHealth.net
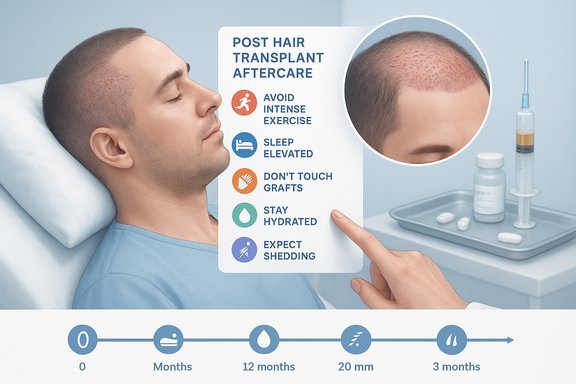 Background / Overview
Background / Overview
The hair restoration market is expanding rapidly: one prominent industry forecast values the global hair transplant market at about US$5.12 billion in 2022, projecting growth to US$23.32 billion by 2030 — a compound annual growth rate in the low‑to‑mid double digits over the forecast window. These figures reflect growing demand, new non‑scalp transplant applications (beard, eyebrow), and an expanding portfolio of adjunctive therapies. Market forecasts are inherently contingent on assumptions about adoption, pricing and regulation, so they should be interpreted as directional rather than definitive. The International Society of Hair Restoration Surgery (ISHRS) practice data shows notable shifts in patient behavior and technique preference: FUE is the dominant surgical approach for many practices, body and facial transplants (beard, eyebrow) are increasing, and about 25% of new patients in a recent ISHRS member survey said the “Zoom effect” (being more camera‑conscious during the pandemic) influenced their decision to seek treatment. The ISHRS census also documents the fast adoption of nonsurgical adjuncts (finasteride, topical minoxidil, PRP) and a growing awareness among patients to prioritize surgeon qualifications. Against that backdrop of rapid growth and innovation, the post‑operative window — the days to weeks after surgery — is fragile. Surgeon advice, patient compliance, and the choice of adjunct therapies can meaningfully affect graft survival and the final cosmetic result. The following sections summarize the five “never do” items highlighted by Dr. Emrah Cinik, expand on the clinical evidence where available, and provide a journalist’s critical appraisal of the strengths, gaps and risks behind the advice. 1. Don’t hit the gym too soon — why exercise matters after a hair transplant
What the advice says
Dr. Cinik and many hair surgeons advise avoiding strenuous exercise for at least the first two weeks after surgery because elevated heart rate, blood pressure and sweating can increase swelling, risk of bleeding and — critically — create micro‑movements at the graft sites that might dislodge fragile follicles during the initial take period. He recommends gentle walking and delaying heavy cardio, resistance training, contact sports and sauna use during the early recovery window.The evidence and physiology
Surgical grafts rely on a brief period of plasmatic imbibition followed by revascularization. In the first 7–14 days grafts lack an established blood supply and small shifts or shear forces can compromise viability. Those physiological facts are well understood in transplant literature and underpin the consensus to avoid activities that markedly increase scalp perfusion or mechanical stress immediately post‑op. While randomized trials specifically testing exercise restrictions are not common, the biological rationale is sound and broadly accepted among hair restoration clinicians.Practical guidance (clinic‑grade)
- Avoid heavy cardio, weightlifting, HIIT, rowing and contact sports for 10–14 days.
- Keep walks short and gentle during the first week; raise your heart rate modestly only after day 7–10 and with your surgeon’s clearance.
- Avoid steam rooms, hot baths and saunas for at least 2–3 weeks because heat and vasodilation increase swelling and bleeding risk.
- If you have a vigorous sweat episode (e.g., from a sudden heatwave), gently rinse the scalp per your clinic’s instructions rather than scrubbing.
2. Don’t sleep flat on your back — managing overnight swelling
The advice and rationale
Post‑operative edema around the forehead and periorbital region is common after hair transplantation. Dr. Cinik recommends sleeping with the head elevated (roughly 30–45 degrees) for the first 5–7 nights to minimize gravity‑driven swelling and avoid friction that could disturb grafts. Travel style cushions or wedges reduce scalp contact and help maintain head position without excessive rubbing.What the literature and experts say
Surgical aftercare protocols from major clinics typically include head elevation to reduce edema and discomfort. Edema rarely threatens graft survival directly, but it can delay healing, increase soreness, and prompt patients to touch or manipulate the treated area — behavior that itself threatens grafts. The elevation recommendation is pragmatic, low‑risk and widely adopted.Practical guidance
- Use a travel neck pillow or an adjustable wedge to keep the head elevated without allowing the graft area to rub on bedding.
- Sleep on your back with gentle head support; avoid stomach sleeping or side sleeping for at least the first 5–7 nights.
- If swelling worsens, call your surgeon; they may recommend short courses of steroids or other measures in selected cases.
3. Don’t “test” the new grafts — hands off, hats off
The core warning
Patients frequently touch, scratch or test the implanted area, especially when it itches or feels odd. Dr. Cinik stresses that grafts are extremely delicate during the first 7–10 days and that repeated contact, pressure, or friction can dislodge follicles and reduce final graft uptake. He also warns against hats, helmets, or tight headwear until the surgeon clears you.Evidence and clinician experience
Graft integrity during the initial take phase is vulnerable to physical disturbance. Multiple clinical guides advise “no touching” and caution about friction from hats, helmets, and even rough pillowcases. There is also published evidence showing that micro‑trauma and contamination increase the risk of crusting and infection. That translates into a clear, pragmatic instruction: minimize any manipulation.Practical guidance
- Resist itching impulses; if your scalp itches, use saline sprays or the topical medications your clinic provided.
- Avoid hats or tight scarves for at least 7–10 days — simple loose head coverings may be allowed after discussion with your surgeon.
- Wear button‑down shirts or zip jackets for the first 2–3 days to avoid pulling garments over your head.
4. Don’t skip hydration and nutrition — nutrition isn’t optional in recovery
Surgeon’s point and why it matters
Dr. Cinik emphasizes that follicles are living grafts requiring energy and building blocks to revascularize and heal; dehydration, alcohol and junk food slow cellular recovery. He recommends increased water intake, lean proteins, vitamin C, zinc and biotin, and abstaining from alcohol for at least a week.What the science supports
Wound healing is energy‑intensive and nutrient responsive: protein supports collagen and tissue repair, vitamin C is essential for collagen cross‑linking, and zinc plays a role in DNA synthesis and immune defense. While there are no large randomized trials specifically linking short post‑op nutrition plans to hair transplant graft take, sound perioperative nutrition is a standard component of surgical recovery across specialties. Dehydration and heavy alcohol use are established to impair wound healing and increase bleeding risk.Practical guidance
- Prioritize daily protein (lean meats, eggs, dairy, legumes) and a colorful array of fruits/vegetables for vitamin C and antioxidants.
- Stay well hydrated (monitor urine color as a simple proxy).
- Avoid alcohol for at least 7–14 days; some surgeons recommend longer abstinence depending on bleeding risk and medications.
- Ask your surgeon about supplements (zinc, vitamin D, biotin) — they can be beneficial but should be tailored to your baseline health and lab values.
5. Don’t panic about early shedding — shock loss is common
The phenomenon
Many patients experience shedding of transplanted hairs around 3–6 weeks post‑op — a process termed “shock loss.” It reflects follicles entering a dormant phase before the new anagen growth cycle begins; new hairs typically appear between 2–4 months and continue maturing over 12–18 months. Dr. Cinik and most clinicians reassure patients that early shedding is usually normal and not an indicator of graft failure.Evidence and timeline
Post‑transplant telogen effluvium (transient shedding) is well documented. The transplanted follicle generally remains viable in the scalp even when the shaft sheds; the clinical challenge is education and expectation management. Patients who panic and then pursue unvetted “fixes” can unintentionally harm grafts or expose themselves to unneeded procedures. Expect gradual regrowth; final density can take up to 12–18 months to fully reveal itself.Practical guidance
- Document photos at standard intervals (baseline, 3 months, 6 months, 9 months, 12 months) — clinicians use serial photos to judge progress.
- Resist rapid additional interventions during the early months unless advised by a qualified surgeon.
- If shedding is accompanied by severe pain, swelling or discharge, contact your clinic — that’s not normal and merits evaluation.
Critical analysis: strengths, gaps and risks in the article’s claims
Strengths — what the surgeon and article get right
- The core aftercare points — avoiding strenuous activity, avoiding friction, elevating the head, prioritizing nutrition, and managing expectations around shedding — align with standard clinical guidance. Those are low‑risk, high‑upside precautions anchored in basic wound‑healing physiology.
- The piece correctly situates hair transplantation as a growing, multi‑modal market with rising patient awareness and interest in both surgical and non‑surgical strategies. The ISHRS practice census and major market reports show clear increases in procedure volumes and adoption of FUE and adjunctive therapies.
Gaps and caveats — where readers should be cautious
- Several emerging adjuncts (notably exosome therapy) are widely marketed but remain largely experimental. Systematic reviews and specialty organizations caution that exosome treatments for hair loss lack standardized manufacturing, large randomized trials and regulatory approval; patients should treat exosome claims with caution and ask for trial data if offered. Exosome products are being sold in some clinics and med‑spas, but the evidence base is currently limited and heterogeneous. Labeling such therapies as “standard” or guaranteed is premature.
- PRP (platelet‑rich plasma) has a stronger evidence base as an adjunct therapy and has been reported in controlled trials to improve early graft survival and hair density when used with transplantation, but studies vary widely in preparation techniques, platelet concentrations and timing. Systematic reviews find consistent directional benefit but emphasize methodological heterogeneity and the need for standardized protocols. Patients should view PRP as a potential booster — not a guaranteed game changer — and should confirm the clinic’s PRP protocol and outcome metrics.
- Market projections (e.g., the Insight Partners report forecasting growth to US$23.32B by 2030) rely on modeling assumptions about adoption, pricing and the regulatory environment. While useful for industry context, forecasts are not clinical evidence and should not substitute for individualized medical advice.
- The article quotes Dr. Cinik’s claim that aftercare determines “up to 70% of the final result.” That framing is compelling but should be treated as a clinician’s heuristic rather than a rigorously quantified fact. Final outcomes are multi‑factorial: surgeon skill, donor hair quality, surgical technique, graft handling, patient biology and aftercare all interact — assigning a single percentage to aftercare oversimplifies the complexity. Flagging such numerical claims as clinician opinion is prudent.
Market and safety risks worth noting
- Medical tourism and variable standards. Rapid market growth has fueled medical tourism and cross‑border clinics. Some offer excellent care; others prioritize volume and cost. ISHRS members and regional surveys warn of “black market” clinics and repair cases from poor‑quality surgeries. Patients must vet providers thoroughly and understand follow‑up and revision pathways.
- Unregulated biologics. Products marketed as “stem cell” or “exosome” therapies often lack robust regulatory oversight. The American Hair Loss Association and specialty reviews urge caution and recommend participation in regulated clinical trials rather than direct‑to‑consumer, unproven offerings.
- Hype vs evidence. Social media, celebrity anecdotes and clinic marketing sometimes outpace scientific evidence. Patients should insist on peer‑reviewed data, clear consent documents, and realistic outcome photos — not only curated marketing images.
Practical aftercare checklist for patients (clinic‑ready)
- Immediate days (0–3)
- Sleep elevated 30–45°; avoid rubbing grafts.
- Follow clinic shampoo and saline protocols; do not aggressively scrub.
- Avoid strenuous activity; take short, gentle walks only.
- Do not smoke or drink alcohol.
- Early recovery (4–14 days)
- Continue head elevation as recommended; avoid hats that press on grafts.
- Avoid heavy exercise, saunas, steam rooms and contact sports.
- Use prescribed medications (antibiotics, analgesics) exactly as directed.
- Weeks 3–8
- Expect shedding; take serial photos and trust the timeline.
- Discuss PRP or adjuncts only with your surgeon; avoid impulsive additional procedures.
- Long term (3–12+ months)
- Maintain scalp health with clinician‑recommended topical or oral therapies (minoxidil, finasteride when appropriate).
- Schedule routine follow‑ups and document progress with standardized photos.
Questions to ask your surgeon before, during and after treatment
- Who will perform the surgery — the named surgeon or a delegated team member?
- What is your documented graft survival or take rate for this technique and patient type?
- If you offer PRP or exosome therapy, can you share the protocol, platelet counts or product lot documentation and peer‑reviewed evidence?
- What is the written aftercare plan (exercise, sleep, dressing, showering) and how do you handle complications?
- If results are unsatisfactory, what is the clinic’s revision policy, timeline and associated costs?
Final verdict: sensible caution, realistic expectations, and where the field is headed
The five “never do” rules outlined by Dr. Emrah Cinik — avoid early strenuous exercise, sleep elevated, don’t touch or press grafts, support healing with nutrition/hydration, and accept early shedding as normal — are practical, low‑risk and aligned with mainstream surgical aftercare. They are valuable because they emphasize patient behavior during the fragile initial weeks when grafts are establishing blood supply. However, patients must navigate an ecology of strong evidence (FUE technique, PRP adjuncts with mixed but promising data) and emerging but unproven trends (exosomes and other regenerative biologics). Market growth and celebrity visibility make hair restoration more accessible — and more heavily marketed — which elevates the importance of patient due diligence, clear outcome metrics, and conservative skepticism of high‑cost, low‑evidence add‑ons. If you’re planning surgery, the most reliable path is a surgeon‑led consultation that documents realistic expectations, an evidence‑based aftercare plan, and a transparent approach to adjunct therapies. Treat immediate post‑op care like tending to a delicate surgical graft: protect it, feed the body what it needs, avoid mechanical stress, and give time for roots to take hold. The combination of qualified surgical technique and disciplined aftercare gives you the best chance of turning a demanding day in the OR into a permanent, natural‑looking improvement.Important note: market forecasts and evolving therapies change quickly — projections like the Insight Partners’ 2030 market figure are useful industry benchmarks but not clinical guidance; experimental biologic treatments such as exosomes remain under study and are not standardized or (in most cases) regulatory‑cleared for hair restoration. Always discuss individual care with a board‑qualified surgeon and confirm any adjunct therapies with peer‑reviewed evidence or an IRB‑approved clinical trial before proceeding.
Source: WorldHealth.net Top Hair Surgeon Reveals: 5 Things You Should Never Do After a Hair Transplant - WorldHealth.net